
Levator Ani Syndrome (LAS) is a chronic pelvic pain condition most commonly experienced as deep, aching rectal pain or a persistent sensation of pressure in the anus. Many patients are told that imaging and lab tests are normal, which can be frustrating and invalidating. However, the absence of findings on scans does not mean the pain is “in your head.” In most cases, the underlying cause is musculoskeletal, involving pelvic floor muscle dysfunction, connective tissue restriction, and nervous system sensitization.
If you have been diagnosed with LAS or are dealing with ongoing anal or rectal discomfort without a clear explanation, understanding how the pelvic floor works can clarify why symptoms develop and how targeted, integrative care may help.
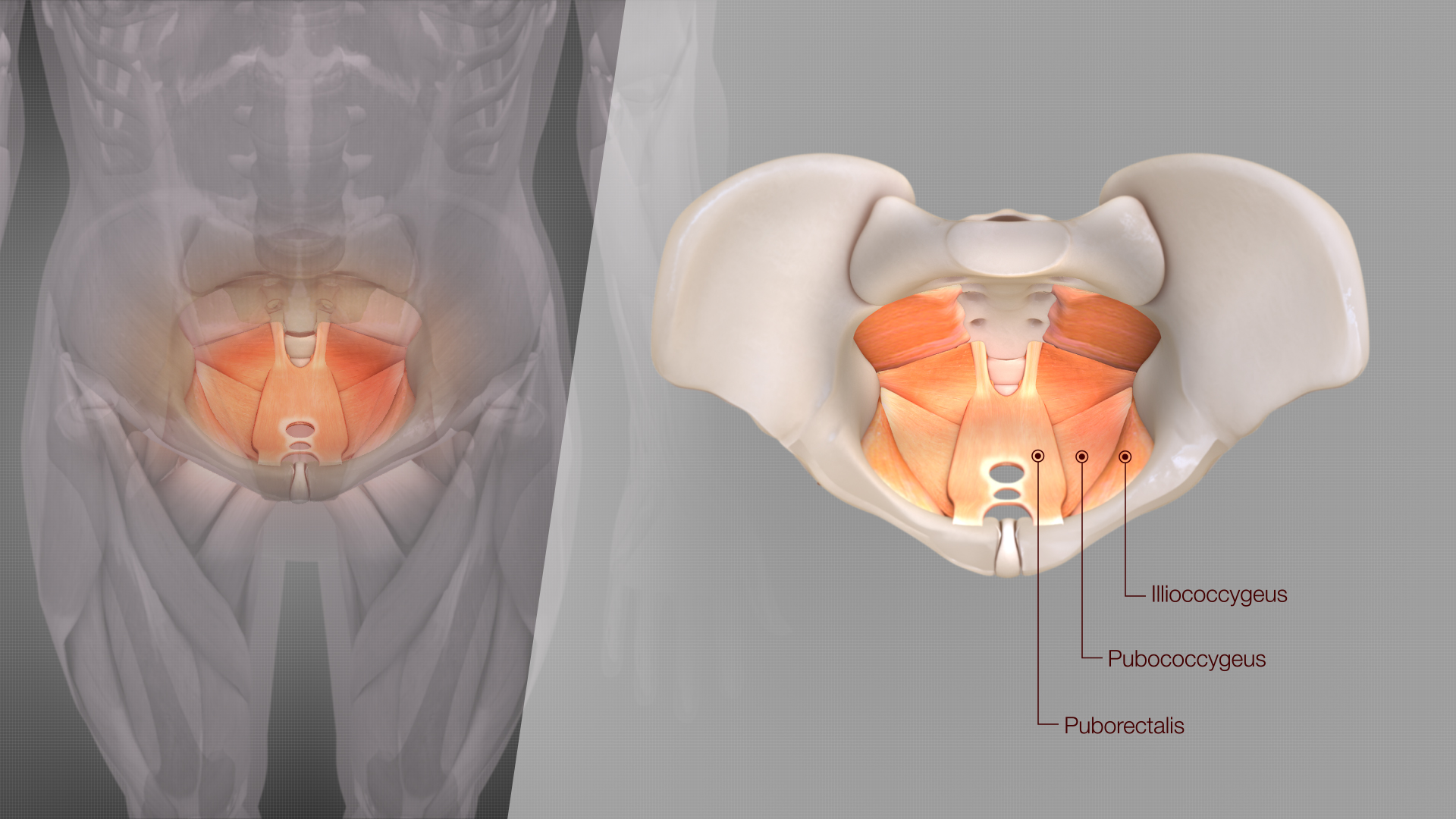
Levator Ani Syndrome is a form of chronic proctalgia, a term used to describe recurring rectal or perineal pain without an identifiable inflammatory or structural disease. It is most often associated with excessive tension or spasm in the levator ani muscle group, particularly the pubococcygeus and iliococcygeus muscles.¹
This pattern of sustained contraction is often referred to as levator spasm. Instead of relaxing appropriately during sitting, bowel movements, or rest, the muscles remain guarded and overactive. Over time, this creates local ischemia, nerve irritation, and referred pain patterns.
LAS is sometimes confused with proctalgia fugax, another functional rectal pain condition. While both involve pelvic floor muscle activity, they differ in presentation.
Proctalgia fugax is characterized by sudden, brief episodes of intense rectal pain that resolve within minutes. Levator Ani Syndrome, by contrast, causes longer-lasting discomfort that may persist for hours or remain present most days. The distinction is important because LAS usually requires direct treatment of pelvic floor muscle dysfunction rather than reassurance alone.
The levator ani muscles work in close coordination with the anal sphincter to support continence, bowel function, and pelvic stability. When the levator ani becomes hypertonic, the anal sphincter often follows suit, leading to increased outlet resistance and pain.
Muscle tension is only part of the picture. The pelvic floor is embedded in a dense network of connective tissue, or fascia, that links the pelvis to the hips, abdomen, spine, and thighs. When fascia becomes restricted due to trauma, surgery, inflammation, or chronic postural strain, it can place constant mechanical stress on muscles and nerves.
These fascial restrictions may not be visible on imaging but can perpetuate pain and autonomic nervous system activation. This is one reason LAS often becomes chronic if treatment focuses only on symptom relief rather than restoring normal tissue mobility.
A diagnosis of Levator Ani Syndrome is typically made based on history and physical examination. During an exam, clinicians may reproduce familiar pain by palpating the levator ani muscles internally or externally. Findings often include tenderness, increased tone, and poor relaxation rather than weakness.
Because LAS is a diagnosis of exclusion, it is important that other causes of rectal pain are ruled out when appropriate. Once structural disease is excluded, treatment can focus on neuromuscular and myofascial contributors.
Some patients find partial relief with conservative strategies such as warm sitz baths, which can temporarily reduce muscle tone and improve circulation. While these approaches may ease symptoms, they rarely address the underlying drivers of chronic levator spasm on their own.
Pelvic floor dry needling is a targeted technique used to release trigger points and hypertonic muscle fibers within the levator ani and related structures. Using a fine, sterile needle, treatment aims to:
Reduce chronic muscle guarding
Because the levator ani is deep and difficult to access externally, dry needling allows for precise intervention when performed by a clinician trained in pelvic floor anatomy and safety.
Acupuncture is often used alongside dry needling to support nervous system regulation, reduce central pain amplification, and improve overall pelvic circulation. In refractory cases of LAS, acupuncture has been associated with meaningful pain reduction, even when other treatments have failed.⁴
Research supports a comprehensive approach to Levator Ani Syndrome:
In my practice, LAS is approached as a whole-system condition rather than a purely local problem. Evaluation includes posture, breathing mechanics, pelvic alignment, and nervous system tone. Treatment plans may include:
Care is individualized and focused on long-term resolution, not temporary symptom suppression.
If you are experiencing persistent rectal or anal pain or have been diagnosed with Levator Ani Syndrome, targeted pelvic floor treatment may be an important next step. Integrative approaches such as dry needling and acupuncture offer evidence-informed options to reduce pain, restore normal muscle function, and calm the nervous system.
Schedule an Appointment or Book a Free Discovery Call




