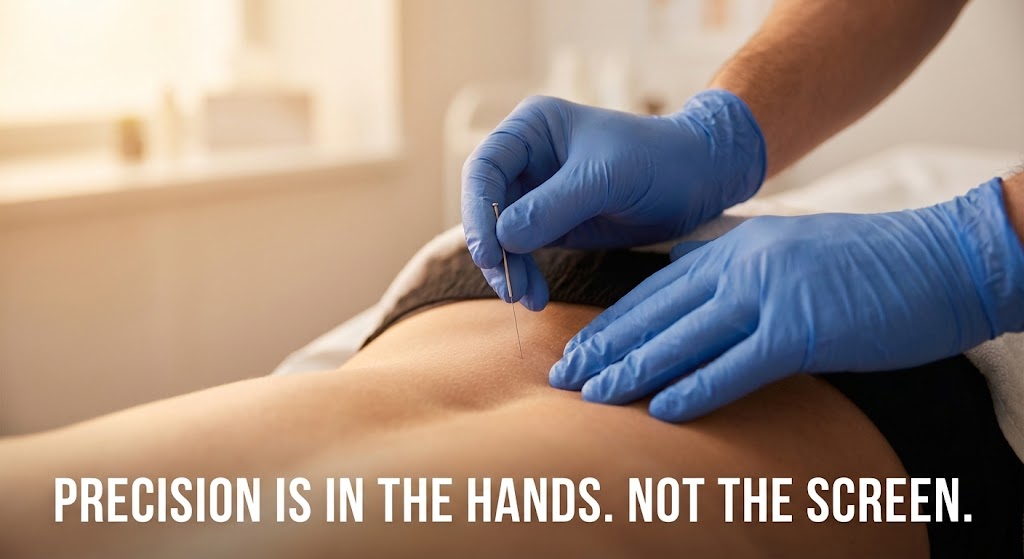
If you are dealing with vulvar pain that makes sitting, exercise, or intimacy feel unpredictable, you have probably wondered whether your pelvic floor is part of the problem. When exploring options through Pelvic Floor Dry Needling for Vulvodynia: A Patients Guide, it helps to understand what this technique can and cannot do, and how it fits into a bigger pelvic health plan. This guide explains why pelvic floor dysfunction can amplify symptoms, what a visit looks like in New York City, and how to choose a qualified provider in Manhattan, Brooklyn, or Queens.
If you are searching specifically in the Upper West Side, look for the same essentials, pelvic health-specific training, consent-forward care, and coordination with your OB-GYN or pelvic floor PT.
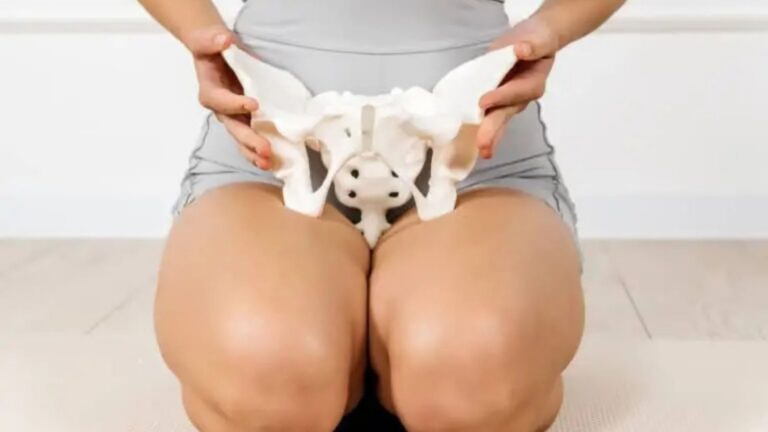
Vulvodynia is chronic vulvar pain that lasts at least three months and is not explained by an active infection or another clear cause. People often describe burning, stinging, rawness, or a “sunburn” sensation, and symptoms may spike with sitting, tight clothing, cycling, or painful intercourse (dyspareunia).
A common driver is an overactive pelvic floor, also called a hypertonic pelvic floor, where muscles stay “on” as a protective response. This guarding can create pelvic floor muscle spasm, restrict fascia and small nerves, and form myofascial trigger points that produce myofascial pain and trigger point referral pain into the vulvar or vestibular region.
You may also hear terms that describe the pattern rather than the cause. Provoked vestibulodynia refers to pain triggered by touch or pressure at the vestibule (for example, penetration, tampon use, or a pelvic exam), while unprovoked vulvodynia describes pain that occurs spontaneously without contact.
Many patients feel confused when symptoms persist even after infections clear. That is often because the nervous system can remain sensitized, and the pelvic floor can stay guarded long after the original irritation is gone, especially with chronic pelvic pain and central sensitization.
In many cases, this ongoing sensitivity reflects peripheral sensitization, where local pain receptors and nearby nerves become more reactive after irritation, and can continue to “over-report” danger even once the original trigger has resolved.
New York City-specific factors can add fuel to the fire. Long commutes, desk work, high stress, breath-holding, and cycling classes can all contribute to pelvic floor tension and symptom flares, particularly when recovery and sleep are inconsistent.
Pelvic floor involvement is not the only cause of vulvar pain, but certain patterns raise suspicion. These signs often show up together, especially when pelvic floor physical therapy finds tenderness or tightness.
A common office test is the Q-tip test, also called the cotton swab test. A clinician gently touches specific points around the vulva and vestibule to perform pain mapping, which helps identify vestibular sensitivity and whether pain is localized or widespread.
A pelvic floor assessment may include an external exam of the hips, abdomen, and pelvic floor region, and sometimes an internal exam to assess muscle tone, trigger points, and coordination. Consent-driven care matters here, so you should expect informed consent, clear explanations, and the ability to pause or stop at any time, especially with trauma-informed care.
Clinicians may also consider whether symptoms match irritation or sensitivity of the pudendal nerve, which helps supply sensation to the vulvar and perineal region. This does not automatically mean a nerve injury, but it can guide decisions about reducing pelvic floor compression, addressing nearby trigger points, and coordinating medical evaluation when neuropathic features are present.
Dry needling uses a very thin filiform needle to target myofascial trigger points, taut bands, and sensitized tissues. It is not acupuncture, and it is taught under a different clinical framework, which is worth reviewing if you are comparing options like dry needling vs acupuncture for pelvic pain whats the difference in ny.
For vulvodynia and related pelvic floor dysfunction, the goal is usually to reduce protective muscle guarding, support pain modulation, and improve tissue mobility around nerves and fascia. In plain terms, the aim is to calm an overactive system, desensitize pain receptors in irritated regions, and restore the ability to contract and relax without spasm.
Manual therapy and manual release can be very effective, especially for superficial tissues and teaching relaxation. Some trigger points and deeper contributors, such as obturator internus or portions of the levator ani, may respond better to the precision of needling when clinically appropriate and performed by a trained pelvic health provider.
You may also hear the term fascial manipulation therapy, which is a hands-on approach aimed at improving glide and load transfer through the fascia that can contribute to pelvic floor guarding. For some patients, clinicians combine fascial work with dry needling to address both tissue mobility and trigger point sensitivity, based on exam findings and symptom response.
Dry needling is rarely a standalone “fix.” The best outcomes usually come when it is integrated into pelvic floor physical therapy, education, down-training, graded exposure, and medical co-management when needed, which is also reflected in clinical discussions you can explore through resources like PubMed.
If you want a service overview, see pelvic floor dry needling and the longer patient resource finding relief from vulvodynia dry needling pelvic floor pain.
Dry needling is often discussed like it is purely “mechanical,” but the effects are both local and nervous-system driven. Understanding the mechanisms helps you set realistic expectations and track meaningful progress.
Trigger point modulation: decreasing local tenderness and referred pain patterns
A trigger point is a sensitive spot in a taut band of muscle that can refer pain elsewhere. By targeting myofascial trigger points, clinicians aim to reduce tenderness, improve blood flow, and decrease trigger point referral pain that can mimic or amplify vulvar pain.
Neurophysiologic effects: down-regulating hypersensitive pain pathways and improving muscle activation/relaxation balance
With chronic pelvic pain, the nervous system can become protective and reactive, which is central sensitization in simple terms. Dry needling can support pain modulation by changing how the nervous system processes threat, and it may help normalize the “on-off” timing of pelvic floor activation and relaxation when paired with down-training and diaphragmatic breathing.
Pelvic floor dry needling tends to make the most sense when the exam points to muscle overactivity and trigger points as meaningful contributors. It can also be useful when progress has plateaued with stretching and manual therapy alone.
You may be a good candidate if you relate to most of the following:
A quality visit should feel organized, collaborative, and measurable. In NYC, it should also be practical, with clear scheduling and coordination options if you are seeing multiple specialists.
A typical step-by-step flow includes intake and history, symptom mapping, and a movement screen that looks at hips, core, breathing, and posture. If indicated, a pelvic floor assessment may follow, and then you and the clinician make a shared decision about whether dry needling is appropriate that day.
During treatment, most people feel a quick pinch or pressure, and sometimes a local twitch response in the targeted muscle. Post-treatment soreness is common and usually lasts 24 to 48 hours, and a short-lived symptom flare can happen if the system is highly reactive.
Aftercare is usually simple and should be tailored to your baseline sensitivity. Many clinicians recommend hydration, gentle walking, heat or ice guidance based on what you tolerate, symptom tracking, and avoiding aggressive stretching if it flares pain.
NYC logistics matter more than people expect. Ask about subway-friendly locations, appointment timing if you commute from Queens or Brooklyn, and how the provider coordinates with your gynecologist, pain management clinician, or pelvic floor physical therapy team.
Vulvodynia care often requires looking beyond the vulvar region. The pelvic floor is influenced by hips, spine, breathing mechanics, and abdominal wall tension.
Commonly addressed areas include:
This often includes the gluteal muscles, since glute tension or weakness can change hip mechanics and increase protective pelvic floor guarding during sitting, walking, and exercise.
Many patients notice change over a short series, but the timeline depends on chronicity, nervous system sensitivity, coexisting conditions, and how consistently the home plan is followed. For some, improvement is rapid; for others, progress is more incremental and linked to nervous system regulation and graded exposure.
A good plan emphasizes reassessment and measurable goals, not just “less tightness.” Useful markers include sitting tolerance, changes in Q-tip test pain mapping, an intercourse pain scale, urinary urgency or urinary frequency changes, and how quickly symptoms settle after a flare.
Dry needling can be very safe when performed by a properly trained clinician using sterile technique and anatomy-specific training. Your provider should also screen for contraindications and explain alternatives if needling is not appropriate.
Some clinics also offer ultrasound guided dry needling, which uses real-time imaging to help confirm anatomy and needle placement when targeting deeper muscles or working near sensitive structures. It is not required and there is no peer-reviewed evidence to support it’s use in this condition, see our post on Do you really need ultrasound guided dry needling?
Common side effects include bruising, mild bleeding at the skin, temporary soreness, and occasional temporary symptom flare. Less common risks include infection, fainting, and nerve irritation, which is why single-use needles, clean technique, and careful anatomical decision-making are essential.
When choosing a provider in New York City, look for pelvic health-specific training and real experience with vulvodynia, not just general dry needling. You also want a consent-forward approach that respects boundaries, explains each step, and supports trauma-informed care.
Dry needling fits best as part of coordinated care. The strongest plans align pelvic floor PT, gynecology, and sometimes pain management or mental health support, especially when central sensitization, anxiety, or fear-avoidance are maintaining symptoms.
If you are also exploring acupuncture, compare approaches and scope using pelvic floor acupuncture midtown for tightness pressure and discomfort. If you are a clinician or want a deeper technical overview, see pelvic floor white paper for clinicians.
A short call or email can save you time and reduce uncertainty. These questions also help you identify whether the clinic has the pelvic health depth vulvodynia often requires.
Some cases need a slower ramp-up before adding needles. That does not mean you cannot improve; it just means the sequence matters.
Dry needling may not be the first step if you have highly reactive pain with frequent symptom flares, an active infection, uncontrolled bleeding risk, or severe anxiety around needles. It may also be premature if symptoms suggest dermatoses, neuropathic pain, or hormonal factors, where medical evaluation should lead and procedures should follow a clearer diagnosis.
Most people do best with a plan that addresses both tissue sensitivity and the nervous system’s protective response. The goal is fewer flares, faster recovery when flares happen, and a return to valued activities like exercise, sitting through meetings, and comfortable intimacy.
A practical example care pathway often looks like this: education about pain mechanisms and triggers, down-training to reduce baseline tone, pelvic floor dry needling to address stubborn trigger points and guarding, and graded exposure to rebuild tolerance. If appropriate, graded exposure can include dilator therapy, progressive penetration strategies, and a paced return to cycling or longer sitting.
Dry needling complements pelvic floor physical therapy when the sequencing is intentional. Many people do well with needling on days when the system is not already flared, followed by gentle mobility, diaphragmatic breathing, and a home plan that reinforces relaxation rather than “stretching harder.”
Common mistakes can slow progress even when you have the right diagnosis. These patterns are fixable, but they often require coaching and consistency.
Local support can make the process easier in New York City. Consider pelvic pain support groups, women’s health physical therapy networks, and coordinated care with local OB-GYNs who routinely manage vulvar pain and vestibular sensitivity.
These examples are simplified and meant to show how treatment pieces can fit together. Your plan should be individualized based on your exam, history, and response.
Provoked vestibulodynia + hypertonic pelvic floor
A patient has sharp pain with tampon use and pelvic exams, plus clear pelvic floor muscle spasm on assessment. After a short series combining down-training, targeted manual therapy, and pelvic floor dry needling to relevant trigger points, Q-tip test mapping shows reduced localized tenderness and the patient tolerates exams with less fear and less pain.
Unprovoked burning + urinary urgency
A patient reports background burning that spikes with stress and also has urinary urgency and urinary frequency. Symptoms improve when treatment combines needling of hip and pelvic contributors, bladder retraining, breathing-based down-training, and stress modulation strategies that reduce flare intensity and shorten recovery time.
Many people improve with pelvic floor physical therapy, especially when an overactive pelvic floor and myofascial trigger points are driving symptoms. Results vary, and combining education, down-training, graded exposure, and targeted tools like dry needling (when appropriate) often improves consistency and durability of results.
The Q-tip test, also called the cotton swab test, uses a cotton swab to gently touch specific areas of the vulva and vestibule to map sensitivity. This pain mapping helps identify localized patterns, track change over time, and guide treatment decisions for vestibular sensitivity and related pelvic floor dysfunction.
There is not one single “new” cure that fits everyone. Evolving options tend to be multidisciplinary, such as coordinated pelvic pain programs, targeted pelvic floor interventions including dry needling in select cases, neuromodulation strategies, and individualized medical management based on hormones, skin conditions, nerve pain features, and central sensitization.
If you are considering pelvic floor dry needling in New York City, the most important next step is a thorough evaluation and a plan that measures outcomes you care about, like sitting tolerance, urinary symptoms, and comfortable intimacy. With the right sequencing and a consent-forward provider, dry needling can be a valuable addition that works well alongside existing pelvic floor physical therapy rather than competing with it.
If you are searching specifically in the Upper West Side, Upper East Side, Midtown Manhattan, Union Square, or Chelsea we are easily accessed by the NYC Subway, look for the same essentials, pelvic health-specific training, consent-forward care, and coordination with your OB-GYN or pelvic floor PT.



