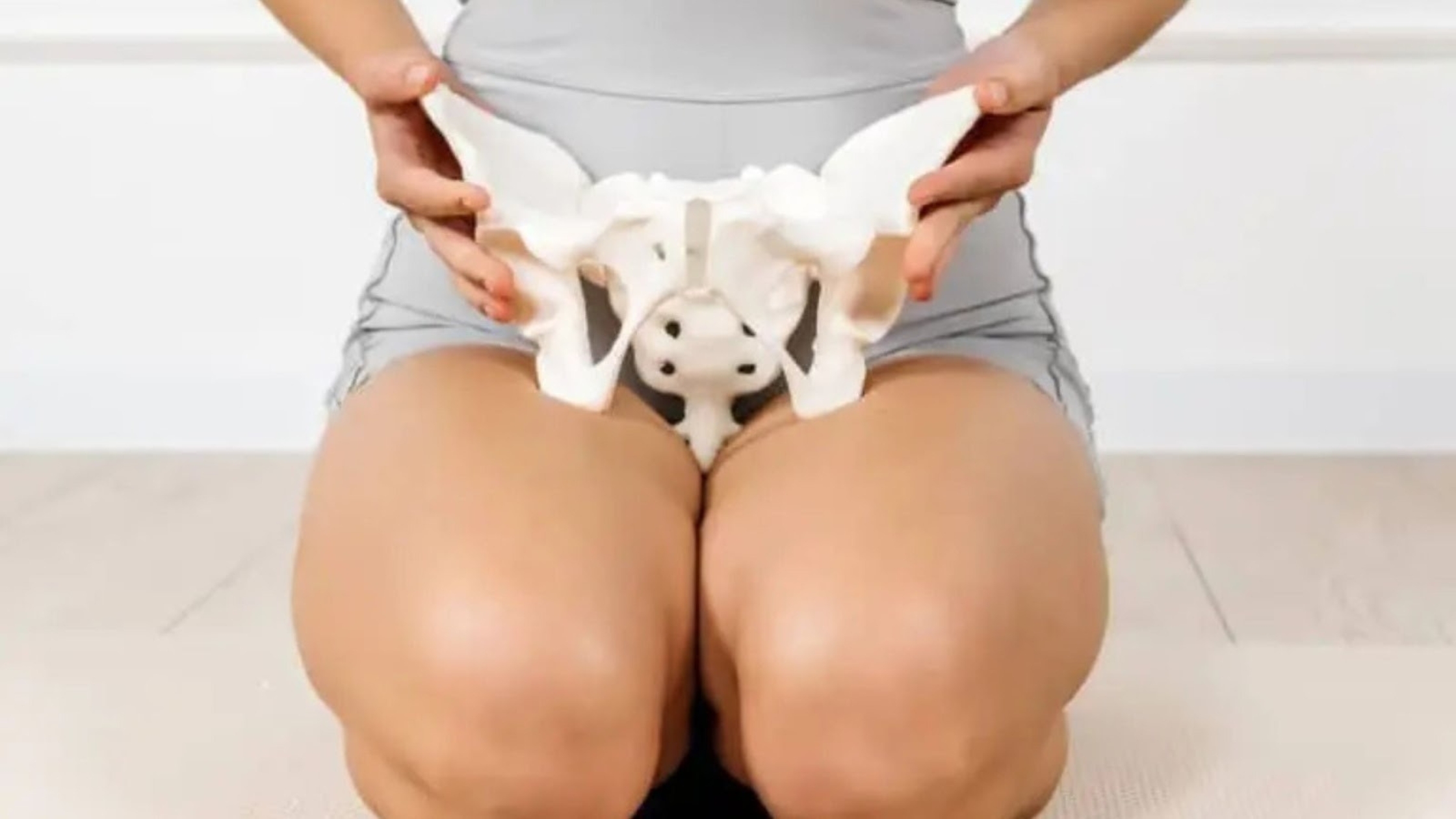
Pudendal neuralgia is a chronic and often life-altering condition involving irritation or entrapment of the pudendal nerve, which supplies sensation and motor control to the pelvic floor, genitals, anus, and perineum. It frequently causes sharp, burning, or electric pain—commonly worsened by sitting and relieved by standing or lying down. Many affected individuals also report difficulties with bowel, bladder, or sexual function.
In my clinical practice, I regularly support patients with pelvic floor-related pain syndromes, including pudendal neuralgia. Pelvic floor dry needling can play an important role in reducing symptoms and improving function. However, this is a complex condition that typically calls for an integrative, multidisciplinary approach involving physical therapy, medical collaboration, and nerve-focused strategies.
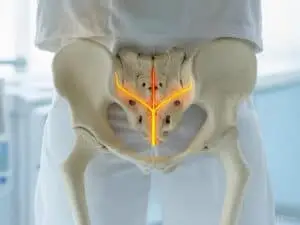
The pudendal nerve originates from sacral nerve roots (S2–S4) and travels through anatomical structures such as the sacrospinous and sacrotuberous ligaments and Alcock’s canal before reaching the perineum. Irritation or compression of this nerve may result from prolonged pressure (e.g., cycling), surgical scarring, trauma, or muscular hypertonicity.
Despite being uncommon, pudendal neuralgia is often misdiagnosed as vulvodynia, chronic prostatitis, or psychological pain—contributing to delayed or ineffective treatment.
Diagnosis is primarily clinical and requires ruling out other conditions. The Nantes Criteria provide a standardized framework for identifying pudendal neuralgia based on symptom presentation, pain distribution, and response to certain movements or positions.¹
Management typically includes:
Many cases of pudendal neuralgia involve hypertonic pelvic floor muscles—such as the obturator internus, levator ani, or coccygeus—that may mechanically irritate the pudendal nerve. Dry needling these muscles can help:
Recent clinical trials have shown that dry needling effectively reduces pain and central sensitization in individuals with chronic pelvic pain, including pudendal neuralgia.² This supports its inclusion in integrative treatment plans, especially when combined with physical therapy and nerve modulation techniques.
For long-term improvement, pudendal neuralgia must be addressed through a collaborative lens. A multidisciplinary strategy—combining physical therapy, dry needling, neuromodulation, and medical or surgical input—is increasingly supported by clinical literature.³⁴ Integrating these tools leads to more sustainable symptom relief than relying on a single intervention.
As a provider specializing in pelvic floor dry needling and integrative pain care, I offer a holistic and trauma-informed approach. In my clinic, you can expect:
Every person is different—and no single modality works for everyone. My goal is to integrate appropriate tools that restore function and empower you in your healing journey.
If you’re dealing with persistent pelvic pain or suspect pudendal neuralgia, I invite you to schedule a consultation. Whether you’re newly diagnosed or searching for answers after multiple failed treatments, we’ll work together to create a personalized, respectful, and effective care plan.
Serving New York City and beyond, with a focus on integrative pelvic floor pain care.