You go down a few subway flights and your knee feels “pressurized,” like something is pushing from behind the kneecap. When working with Vastus Intermedius Trigger Points, that deep knee pressure and stubborn anterior thigh pain often makes more sense than it does under a generic “runner’s knee” label. This guide explains what’s happening, how to self-check safely, and how to combine relief with better load management so symptoms do not keep cycling back.
Trigger points are not the same thing as general muscle soreness after a hard workout. They are more specific, and they tend to behave in repeatable patterns.
A trigger point is typically felt as a taut band with a tender nodule inside it, and pressing it can reproduce a familiar symptom rather than just “ouch, that’s sore.” Many people also notice referred pain, meaning pressure in the thigh can create discomfort that feels closer to the knee.
General soreness is usually diffuse and improves predictably with time and light movement. Trigger points are more load sensitive, meaning stairs pain, prolonged sitting, or repeated knee bends can spike symptoms even when the muscle “should be warmed up.”
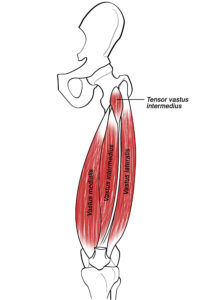
The vastus intermedius sits deep under the rectus femoris, so it is harder to palpate than the vastus lateralis or vastus medialis. Because it is not easy to “find,” it often gets ignored in favor of more obvious structures near the patella and patellar tendon.
Its symptom patterns also overlap with patellar tendinitis, patellar tendinopathy, and patellofemoral pain. Many people get treated only at the front of the knee even though the driver is a compressive load problem that the deep quadriceps is reacting to.
New York City loads knees in a very specific way. Subway stairs, long walking commutes, cycling, and long desk hours create a mix of repeated knee flexion plus prolonged sitting that can sensitize the anterior thigh and knee.
Downstairs is often the tipping point because it increases compressive load and demands more control of tibial position. Add in a heavy bag and rushed pacing in Manhattan, and the knee may feel “fine until it suddenly isn’t.”
Treating this area is not only about chasing anterior knee pain. People often report changes in knee tracking, reduced deep pressure behind or under the patella, and better tolerance to prolonged sitting and stairs.
That matters because it suggests the vastus intermedius behaves like a deep stabilizer that reflects joint mechanics and compressive load. In other words, it can be a marker of how the knee is being loaded, not just how strong the quadriceps are.
The quadriceps group includes rectus femoris, vastus medialis, vastus lateralis, and vastus intermedius. The intermedius is the deepest of the four, and its role is often underestimated.
The vastus intermedius lies on the anterior femur and is covered by rectus femoris. Its fibers contribute to the quadriceps tendon, which attaches to the patella, and force continues through the patellar tendon to the tibial tuberosity.
Because of this linkage, tension or sensitivity in the deep quadriceps can be felt as knee stiffness or a “pressure” sensation near the kneecap. That does not automatically mean tissue damage at the patellar tendon, even if the pain feels close by.
Yes, it contributes to knee extension, but clinically it often behaves like a deep stabilizer. When compressive load rises, or when knee tracking is off due to hip rotation or tibial rotation issues, it can tighten as a protective buffer.
This is why someone can have strong-looking quads and still feel limited on stairs or after prolonged sitting. The problem is not always output strength, but tolerance to compressive mechanics and sustained flexion.
Trigger points can be active or latent, and that distinction changes how symptoms show up day to day. Both can contribute to myofascial pain syndrome when they persist and start influencing movement.
Active trigger points reproduce your familiar complaint when pressed. They may also create referred pain that feels like it spreads toward the knee, or creates a deep ache along the anterior thigh.
People often describe an “aha” moment when pressure in mid-thigh triggers the same deep knee pressure they get on stairs. That reproduction is one reason clinicians pay attention to trigger points rather than only chasing the pain site.
Latent trigger points are tender, but they do not always reproduce the exact familiar pain. They often show up as stiffness, limited tolerance to prolonged sitting, or a subtle change in gait mechanics such as avoiding knee bend on one side.
They can still matter because they alter movement and load distribution. Over time, that can feed into patellofemoral pain patterns or recurring anterior knee pain with training.
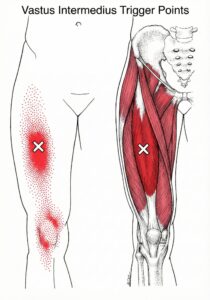
The vastus intermedius can create a recognizable cluster of symptoms, but it rarely shows up alone. It often overlaps with patellar tendon irritation, quadriceps tendon sensitivity, or hip and ankle drivers.
Common reports include anterior thigh pain that feels deep rather than superficial, knee stiffness, and a “dense pressure” behind or under the patella. Many people notice stairs pain, especially downstairs, or discomfort after prolonged sitting that improves after a few minutes of walking.
Symptoms can fluctuate with workload more than with single movements. That is a hallmark of load sensitivity rather than a single injured structure.
Because of its anatomy and referral patterns, this can mimic patellar tendinitis or patellar tendinopathy. It can also blend into runner’s knee and broader patellofemoral pain, especially when knee tracking is inconsistent.
In some cases, people interpret it as meniscus irritation or even MCL symptoms because the knee feels “tight” or “caught” during flexion. That is why a differential matters, particularly if symptoms include swelling, locking, or instability.
A classic pattern is someone who can produce force but cannot tolerate compressive tasks. Downstairs, deep knee bend positions, and long sits tend to flare symptoms because they increase compression and demand control.
This is also where the “deep stabilizer” idea helps. The muscle may be overactive to protect the joint when hip control, tibial position, or ankle mechanics are not distributing load well.
In New York City, the triggers are often predictable. Running loops in Central Park or Prospect Park, hill repeats on bridges, spin classes with high resistance, and simply stacking high daily step counts can push compressive load beyond tolerance.
The tricky part is that none of these are “bad.” The issue is how quickly volume ramps, and whether recovery and mechanics keep pace.
These checks are meant to guide your next step, not to diagnose an injury. Stop if you feel sharp pain, worsening swelling, or any sense of instability.
Sit or lie down with the knee slightly bent to relax the quadriceps. Using fingertips or knuckles, explore the mid-thigh area and compare sides, noticing whether one side has a deeper, more specific tender spot.
Pay attention to whether pressure reproduces your familiar deep knee pressure or anterior knee pain. Reproduction does not prove a cause, but it is a useful clue to discuss with a clinician.
Use a simple step-down test from a low step, moving slowly and tracking how the knee feels during and after. Note where symptoms show up, such as under the patella, along the patellar tendon, or deeper in the knee.
Also track what happens after prolonged sitting, such as a 30 to 60 minute desk block. Location and behavior over time often reveals more than a single pain score.
Trigger points can coexist with other conditions. If your symptoms do not match a typical myofascial pattern, get evaluated.
Seek medical evaluation if you have visible swelling, locking, true instability or giving way, fever, night pain, or recent trauma. Those signs can point to joint injury, infection, or other conditions that need prompt care.
Also get assessed if pain is rapidly worsening or you cannot bear weight. A trigger point problem is usually uncomfortable, but it typically does not create dramatic swelling or mechanical locking.
A thorough differential often includes patellofemoral pain, patellar tendinopathy, quadriceps tendinopathy, and IT band-related pain. Hip referral and lumbar referral can also present as anterior thigh pain or altered knee sensations.
This is where a good exam matters, because treatment changes depending on whether the primary driver is tendon load, joint irritation, referred pain, or myofascial pain syndrome. Many people have more than one contributor, and the plan should reflect that.
Relief is useful, but it is not the finish line. Trigger point release can reduce sensitivity, yet it will not hold if gait mechanics and load management stay the same.
If hip rotation control is limited, the knee often collapses inward and increases tracking stress. If tibial rotation and tibial position are not controlled, the knee can feel “twisty” under load even when the quads are strong.
If ankle mechanics limit dorsiflexion, the body often steals motion from the knee and hip, increasing compressive load at the patellofemoral joint. These are common reasons why the vastus intermedius keeps re-engaging after manual therapy.
For 7 to 14 days, reduce compressive volume rather than eliminating all activity. That can mean fewer subway stairs, avoiding deep knee bends, lowering cycling resistance, and limiting downhill running.
During desk work, use movement breaks every 30 to 45 minutes. Even 60 to 90 seconds of easy walking, mini-squats to a chair, or gentle knee extensions can reduce stiffness from prolonged sitting.
Once symptoms calm, rebuild capacity with progressive loading. The goal is not to “stretch it out,” but to increase tolerance of the quadriceps and improve hip control so the knee tracks better under load.
Use pain-guided dosing. A mild discomfort during exercise that settles within 24 hours is often acceptable, while sharp pain or escalating next-day stiffness suggests you did too much.
NYC makes perfect rehab consistency hard, so micro-doses work well. Two to five minutes before leaving the apartment, one short set after commuting, and a brief evening session can add up without requiring a full gym block.
Also treat stairs like training volume. If you have to climb them, reduce other compressive work that day so total load stays manageable.
Self-release can help modulate tone and pain sensitivity, especially when paired with movement. The key is to avoid turning it into an aggressive digging contest that irritates the knee.
A foam roller works well for the superficial quadriceps, including rectus femoris, vastus lateralis, and parts of vastus medialis. For more targeted work, use a massage ball against a wall so you can control pressure and angle without bracing hard through the knee.
Avoid aggressive digging directly above the patella or into the quadriceps tendon if it flares patellofemoral pain. If your knee feels more “pinchy” after rolling, lighten up and shorten the session.
Pick one to three tender areas and apply steady pressure for 30 to 60 seconds per spot. Do 1 to 2 rounds, then stop.
Re-test something meaningful, such as a sit-to-stand, a few stairs, or a gentle step-down test. If there is no change, more pressure is rarely the answer, and you may need a different lever like load reduction or strength work.
The vastus intermedius often tightens when other joints are not sharing load. Improving control in the hip and ankle can reduce knee tracking stress and lower compressive load where it does not belong.
Prioritize hip abductor and external rotation control so the femur does not collapse inward. Good options include side-lying hip abduction, banded lateral walks, and controlled single-leg hinges with a light reach.
When you step down or squat, watch for knee valgus and correct with slower tempo and smaller range. Better hip control often reduces the feeling that the knee is “grinding” or drifting off track.
If dorsiflexion is limited, try a gentle knee-to-wall drill and calf strengthening rather than only stretching. Pair it with foot control work, such as short-foot holds or slow calf raises, to improve pronation control.
These changes can reduce unwanted tibial rotation during walking and stairs. Less tibial rotation often means less stress on the patellofemoral joint and less need for the deep quadriceps to brace.
Because this muscle behaves like a deep stabilizer, strength work should emphasize control and tolerance under compression. Start with isometrics, then build toward slow, controlled knee-bend patterns.
Isometrics can reduce pain sensitivity while keeping quadriceps output high. A wall sit at a tolerable knee angle or a Spanish squat setup can be effective, especially for anterior knee pain patterns.
Aim for 3 to 5 sets of 20 to 45 seconds, resting 60 to 90 seconds between sets. Keep discomfort mild to moderate and avoid angles that create sharp patellar tendon pain.
Move to step-downs with a slow lower and light fingertip support if needed. Then add split squats, focusing on a quiet knee path and steady hip control.
As tolerance improves, introduce controlled knee-over-toe work in small doses, such as a shallow heel-elevated squat or a slow forward lunge. The goal is graded exposure to compressive load, not forcing range on day one.
When self-care is not enough, clinical work can speed up symptom modulation and clarify what is driving the problem. The best results usually come from pairing hands-on work with movement retraining.
A good clinician does not only chase a sore spot. They look at tone normalization in a deep stabilizer muscle, then check upstream and downstream drivers like hip control, tibial mechanics, and gait mechanics.
That is important because the vastus intermedius often becomes overactive when the knee is trying to stabilize against poor rotation control. When tone drops after treatment, the underlying movement strategy becomes easier to see and fix.
Dry needling is typically used within a musculoskeletal framework to address trigger points and myofascial pain syndrome. Acupuncture comes from a different framework, but it can also reduce pain sensitivity and improve tolerance to movement for some patients.
Either approach is most useful when it is integrated with rehab. If you only “turn down the alarm” but keep the same stair volume and mechanics, symptoms often return.
If you are exploring local options, this resource can help: dry needling trigger point acupuncture in nyc.
Trigger point therapy can include manual therapy, sustained compression, and myofascial release techniques. For a deep muscle like vastus intermedius, clinicians often work through the superficial quads and use positioning to access deeper layers without excessive force.
A good session should change something functional. That might be improved step-down mechanics, less knee stiffness after sitting, or a clearer sense of knee tracking during stairs.
In Manhattan, many Midtown and Upper West Side clinics offer dry needling, acupuncture, and manual therapy under one roof. Brooklyn also has a growing number of rehab studios that combine strength coaching with hands-on care.
For more complex cases, hospital-based sports medicine and pain management practices can evaluate whether imaging, medication, or trigger point injections are appropriate. The setting matters less than whether the plan includes re-testing and progressive loading.
A solid plan is not “come in forever and roll your quads.” It is a structured process that measures change, builds capacity, and reduces recurrence.
Re-testing should be built into each visit and each phase of self-care. Useful re-tests include a short stair bout, a timed prolonged sitting tolerance check, step-down test quality, and your perceived knee tracking.
If the intervention helps but re-tests do not change, the plan needs adjustment. That might mean changing exercise dosage, addressing ankle dorsiflexion, or modifying running volume.
Load management should be explicit and week-to-week. That includes running volume, hills and bridges, cycling resistance, and stair exposure.
A practical rule is to change only one major variable at a time. If you add hill repeats and also increase spin resistance and also take more stairs, you lose the ability to identify the real trigger.
Trigger point injections are not a first-line step for most active people. They can be useful in specific situations, but they should not replace movement work.
Clinicians usually consider trigger point injections when persistent myofascial pain does not respond to conservative care like exercise, manual therapy, myofascial release, and dry needling. They may also be considered when pain limits participation in rehab despite good programming.
The decision should be individualized, especially if there are overlapping tendon or joint issues. A thorough exam helps avoid treating a trigger point when the main driver is something else.
Injections can reduce sensitivity, but they do not change mechanics. Pairing them with movement retraining and strengthening is what reduces recurrence.
The goal is to keep the knee stable under compressive load without the deep quadriceps staying on high alert. That usually means better hip rotation control, improved tibial position during loading, and ankle mechanics that allow clean knee bend.
Most setbacks come from treating the symptom location instead of the loading pattern. The vastus intermedius is often a messenger, not the villain.
It is easy to focus only on the patella, patellar tendon, or quadriceps tendon because that is where the discomfort is felt. But deep anterior thigh pain and pressure-like knee symptoms often reflect compressive load and knee tracking problems.
Treating the front of the knee alone can miss the deeper stabilizer response. That is why some people improve briefly, then relapse as soon as stairs and sitting stack up again.
More pressure is not always better. Aggressive rolling can irritate patellofemoral pain and make the knee feel more sensitive during stairs and sitting.
A better strategy is short, controlled self-release followed by a re-test and then a small dose of strength work. If the knee feels worse after your session, reduce intensity and focus on load management.
If hip control is poor, the knee will keep collapsing inward and the deep quadriceps will keep bracing. If ankle dorsiflexion is limited, the knee often takes extra compressive load during squats, stairs, and walking.
Also consider gait mechanics, especially if you recently changed shoes, increased speed, or returned after injury. Small changes in tibial rotation and tibial position can be enough to keep symptoms simmering.
The key takeaway is that the vastus intermedius is rarely “the problem.” It is often a marker of how the knee is being loaded.
Relief methods like trigger point release, trigger point therapy, myofascial release, manual therapy, dry needling, or acupuncture can help normalize tone. Lasting results come from fixing the load with smarter volume, better hip and ankle mechanics, and progressive strength.
A runner in NYC reports strong superficial quads and consistent training, but gets deep knee pressure after bridge runs and repeated subway stairs. Palpation finds tenderness deep in the mid-thigh, and a step-down test shows shaky control and mild knee valgus.
Dry needling and targeted release reduce the “tracking weirdness” and improve stair comfort for a few days. The lasting change comes from isometrics, slow step-down control, hip stability work, and graded stair exposure that respects weekly load management.
Start by reducing compressive triggers for 1 to 2 weeks, especially stairs volume, deep knee bends, and long sitting without breaks. Add gentle self-release with a foam roller for the superficial quadriceps and a massage ball against a wall for targeted pressure, then re-test stairs or sit-to-stand.
Next, rebuild tolerance with isometrics such as wall sits or Spanish squat variants, then progress to controlled step-downs and split squats. Address hip control, hip rotation, and ankle mechanics so the knee is not forced to absorb extra compressive load.
Because it is deep under rectus femoris, you usually “target” it best through function rather than aggressive poking. Knee-extension isometrics, controlled squats, step-down patterns, and pain-guided progressive loading are often more effective than trying to dig directly into the muscle.
If symptoms persist, clinician-guided dry needling or manual trigger point therapy can access deeper tissue safely and help clarify whether the muscle is acting as a protective stabilizer. The key is pairing that with mechanics work so the change holds.
The vastus intermedius sits deep on the front of the thigh, underneath rectus femoris. It attaches along the anterior femur and contributes to the quadriceps tendon at the knee, which connects to the patella and continues through the patellar tendon to the tibial tuberosity.
Use gentle self-release on the outer quadriceps with a foam roller or massage ball, and reduce aggravating volume like hills, heavy cycling resistance, or high stair exposure for a short period. Then strengthen hip abductors and external rotators to improve hip control and reduce stress that can drive lateral thigh tightness and altered knee tracking.
Add slow step-down work to improve control of tibial rotation and tibial position. If pain persists, spreads to the outer knee, or includes swelling or instability, get an evaluation to rule out IT band-related pain or other contributors.
Deep knee pressure, anterior thigh pain, and stairs pain that do not match a simple tendon story often involve the deep quadriceps and how it responds to compressive load. When you approach the vastus intermedius as a deep stabilizer, relief strategies like trigger point release and dry needling become more useful, but only when they are paired with hip, knee, and ankle mechanics plus progressive loading. With the right mix of symptom modulation, re-testing, and NYC-friendly load management, most people can improve knee tracking and regain confidence on stairs, long walks, and training without constantly chasing the front of the knee.