
Back pain often affects more than movement alone. Many people in New York City notice that when back pain persists, daily mobility gradually decreases, and sleep quality begins to change. Stiffness during the day and disrupted rest at night are frequently linked, even when pain levels fluctuate or imaging results appear unchanged.
For patients seeking clarity rather than reassurance, understanding how Acupuncture Helps Back Pain NYC patients improve mobility and support better sleep requires a closer look at how the musculoskeletal and nervous systems interact. Back pain is rarely isolated to a single structure, and sleep disruption is not simply a nighttime problem.
This article explains how acupuncture is used clinically to address back pain that interferes with movement and sleep. The focus is on evidence-informed care, clinical reasoning, and realistic expectations, not guarantees or generalized treatment claims.
Mobility and sleep are regulated by overlapping systems. When back pain becomes persistent, these systems often influence one another in predictable ways.
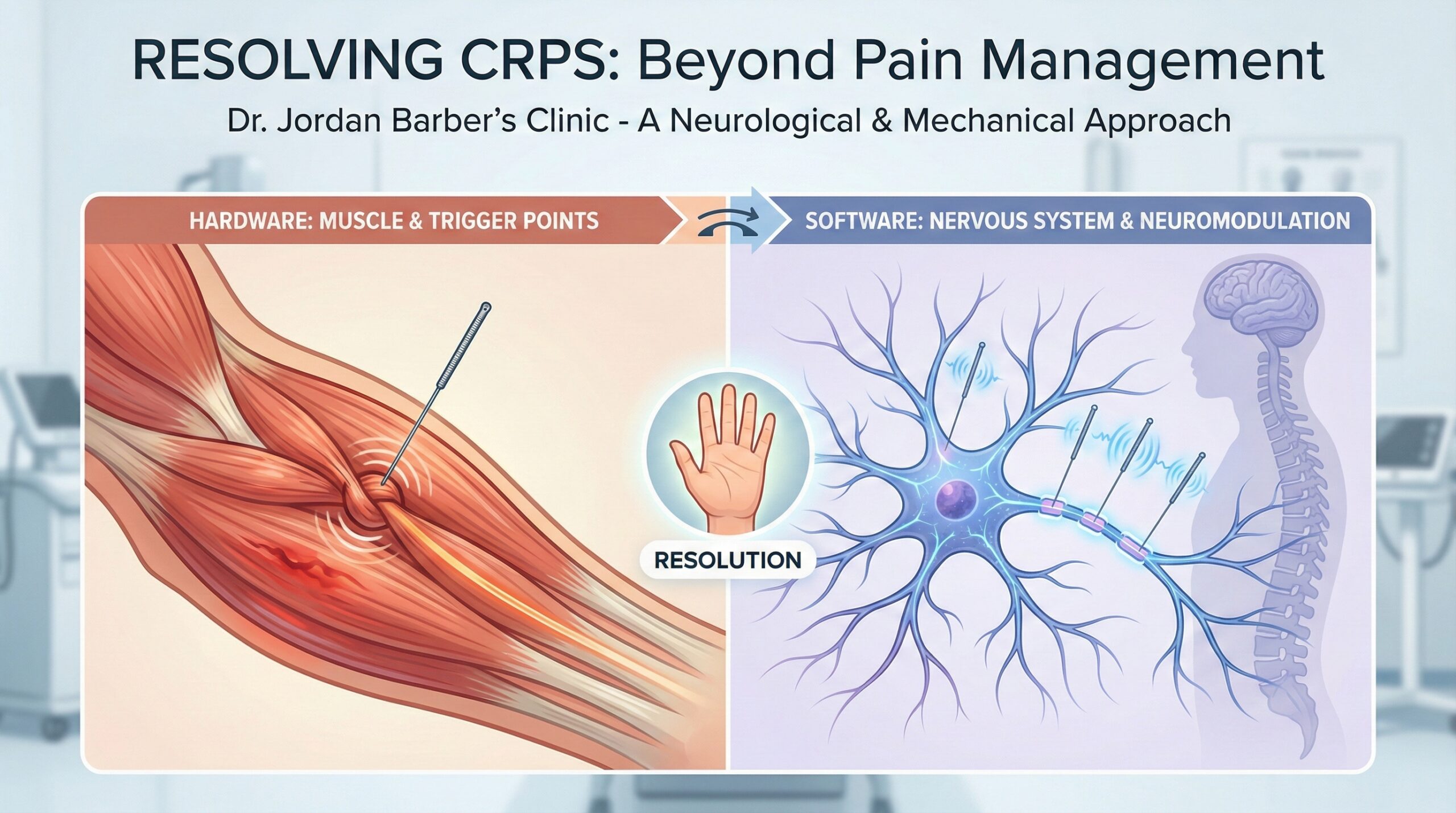
Musculoskeletal restriction alters movement patterns and reduces the body’s ability to distribute load efficiently. Increased nervous system sensitivity can amplify normal sensory input, making both movement and rest less comfortable. Prolonged static postures, common in desk-based and transit-heavy NYC routines, place sustained load on spinal structures and supporting muscles.
Pain intensity alone does not explain mobility loss or sleep disruption. Many individuals report limited movement or poor sleep even when pain is intermittent or moderate. This highlights the role of nervous system regulation, muscle tone, and joint mechanics beyond pain severity alone.
Mobility limitations develop gradually through changes in how the body adapts to discomfort.
Reduced spinal and pelvic joint motion limits normal bending, rotation, and transitional movements. Muscle shortening and altered coordination reduce available movement options and efficiency. Over time, guarded movement patterns develop as the nervous system prioritizes protection, even when tissue damage is minimal.
Imaging findings often fail to explain functional limitations. Disc bulges, degenerative changes, or arthritis may be present without significant symptoms, while individuals with minimal imaging findings may experience notable movement restriction. This disconnect underscores the importance of functional assessment over structural assumptions.
Sleep requires the ability to maintain supported positions with minimal sensory disturbance. Back pain can interfere with this process in several ways.
Difficulty maintaining comfortable sleep positions is common, especially when spinal stiffness limits positional changes. Increased sensory input from irritated tissues can disrupt the ability to settle into rest. Reduced movement variability overnight may lead to morning stiffness and discomfort.
Sleep quality and pain perception influence one another. Poor sleep can heighten pain sensitivity, while persistent pain can fragment sleep, creating a reinforcing cycle that affects daily function.
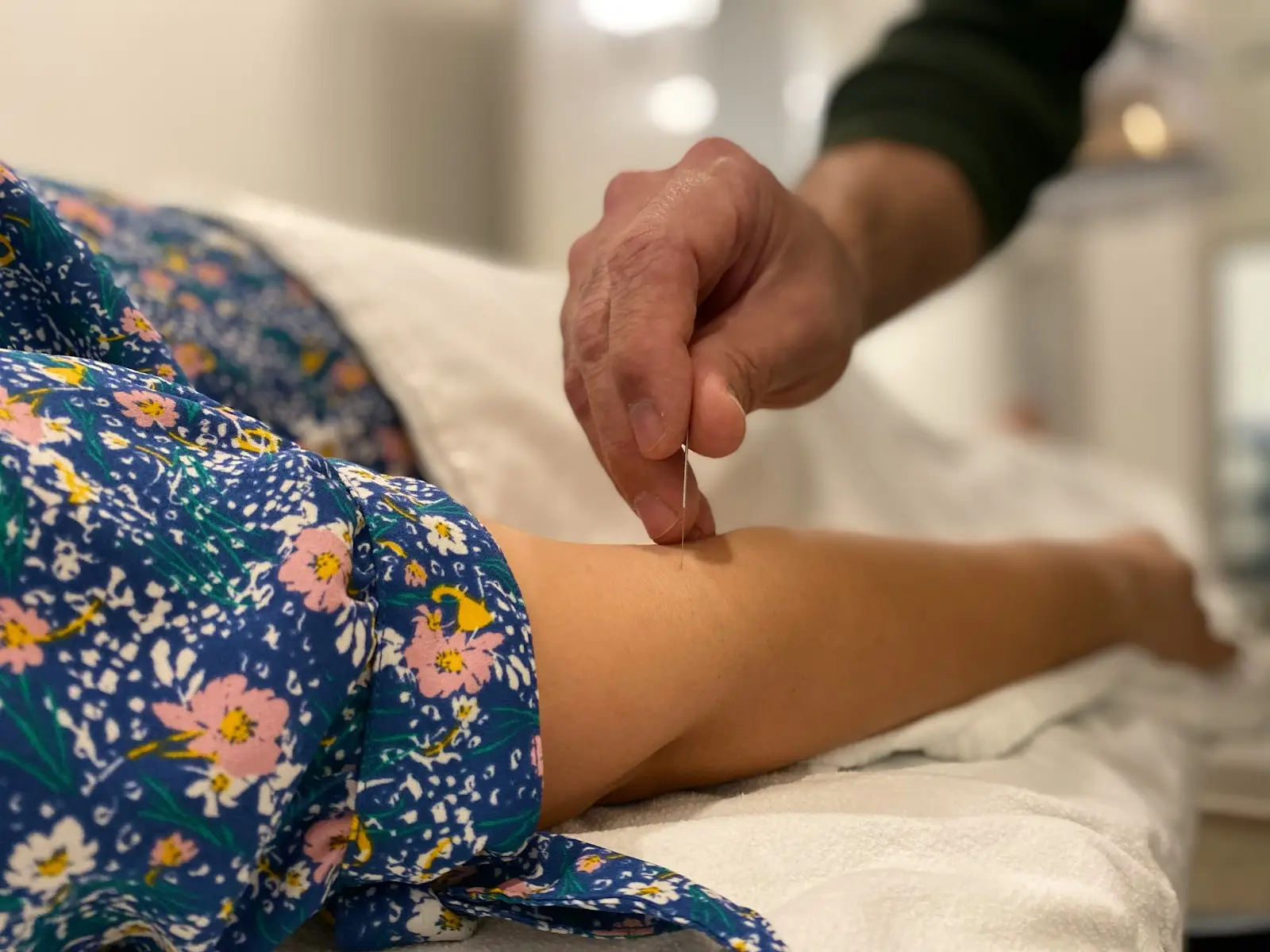
Acupuncture is a licensed medical profession under New York law. In a clinical back pain setting, it is applied based on assessment findings rather than standardized protocols.
Treatment decisions are guided by symptom behavior, movement testing, and neurologic findings. Acupuncture and dry needling are used as clinical tools within a broader diagnostic and reasoning process, not as standalone solutions.
The intent is to influence contributing systems, including muscle tone, joint movement tolerance, and nervous system sensitivity, rather than focusing solely on pain relief.
When applied appropriately, acupuncture may support mobility by influencing factors that limit movement.
Modulation of pain signaling can reduce protective inhibition that restricts motion. Reduction of excessive muscle tone may allow joints to move through a greater range with less resistance. Improved tolerance for joint and soft tissue loading can support daily activities such as walking, bending, and sitting transitions.
These effects do not alter spinal structure. Instead, they influence how the nervous system regulates movement and load distribution.
Research suggests acupuncture may provide short-term symptom modulation for certain back pain populations. Some studies report improvements in function alongside pain reduction.
However, important limitations exist. Treatment methods vary across studies, making comparisons difficult. Follow-up periods are often short, limiting conclusions about long-term outcomes. Results do not apply uniformly across all types of back pain.
Individual assessment remains critical when interpreting research findings. Clinical response depends on whether pain is driven primarily by muscle guarding, joint restriction, nerve sensitivity, or combined factors.
When pain interferes with sleep, addressing contributing factors may indirectly support rest.
Reduced discomfort during position changes can make it easier to maintain supported sleep postures. Improved regulation of muscle tone may reduce nighttime stiffness. Modulation of nervous system activity may help some individuals transition into rest more comfortably.
These effects are supportive rather than corrective. Acupuncture does not directly treat sleep disorders but may influence sleep when pain is a contributing factor.
Some research suggests acupuncture may support sleep quality when pain contributes to sleep disruption. Evidence does not support universal or guaranteed improvements in sleep.
Sleep outcomes are influenced by daytime movement patterns, posture, workload, and environmental factors. Addressing these contributors remains essential for sustained improvement.
Muscle guarding is a frequent contributor to both movement restriction and sleep discomfort.
Lumbar stabilizers may remain persistently active. Hip and pelvic musculature often contribute to spinal loading patterns. Paraspinal muscle groups may maintain protective tension that limits movement variability.
Prolonged sitting and limited movement diversity, common in NYC work environments, reinforce these patterns over time.
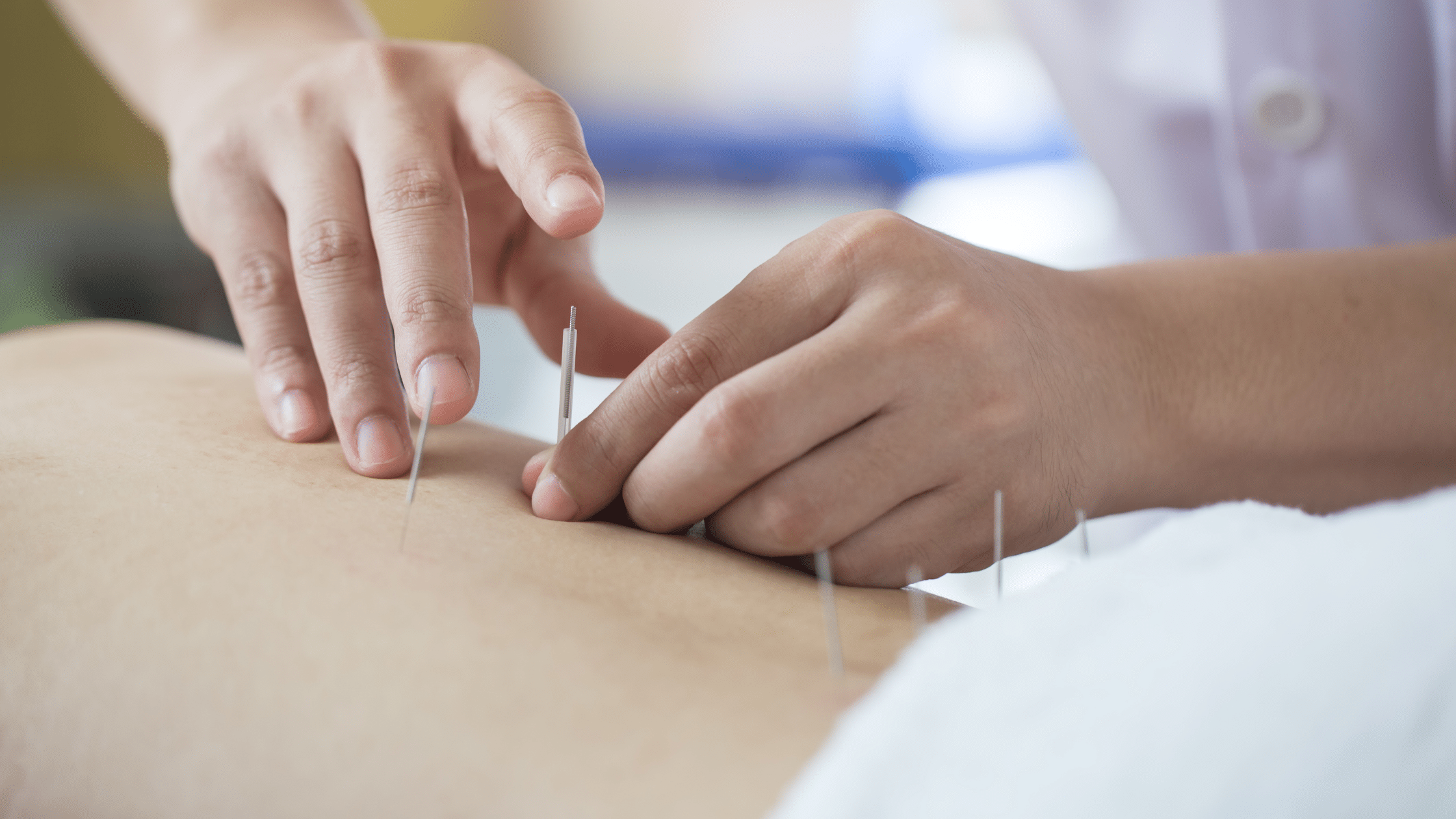
Acupuncture and dry needling may be used to target specific myofascial contributors identified during assessment. Treatment aims to reduce unnecessary guarding and improve tissue tolerance rather than simply relaxing muscles.
Ongoing reassessment ensures that care remains responsive to changes in symptoms and function.
Determining where to begin requires a structured evaluation rather than an assumption.
Movement analysis identifies restrictions and compensations. Neurologic screening assesses sensitivity and referral patterns. Response to load and position changes helps clarify which systems are driving symptoms.
Treatment frequently extends beyond the area of reported pain because contributors often originate elsewhere in the movement system.
Care typically begins with an initial evaluation and planning phase. Short-term response is monitored to determine whether acupuncture is influencing mobility or sleep-related symptoms.
Adjustments are made based on clinical findings rather than predetermined schedules. Indefinite treatment plans are avoided when progress is limited or absent.
Acupuncture is generally well-tolerated when provided by licensed professionals. Temporary responses such as mild soreness or fatigue may occur.
Coordination with other healthcare providers is appropriate when indicated. Acupuncture complements, rather than replaces, medical care.
In some situations, further medical evaluation is necessary before continuing or initiating acupuncture care. Progressive neurologic symptoms, recent trauma, or unexplained systemic changes may indicate conditions that require additional testing or coordinated care.
Recognizing these signs early helps ensure that treatment decisions are appropriate and safe. When red flags are present, timely referral to the appropriate healthcare provider supports accurate diagnosis and effective management.
Progress is evaluated clinically through changes in movement tolerance, symptom behavior, and sleep quality. Acupuncture may be used alone or alongside other care depending on assessment findings.
If mobility or sleep does not change, reassessment guides next steps. Treatment plans evolve based on response rather than fixed expectations.
How is progress evaluated clinically?
Progress is assessed through changes in movement tolerance, symptom behavior during daily activities, and reported sleep quality rather than pain scores alone.
Is acupuncture used on its own or combined with other care?
Acupuncture may be used alone or alongside other approaches, depending on assessment findings and how symptoms respond over time.
What happens if mobility or sleep does not change?
If meaningful change is not observed, reassessment guides next steps. Treatment plans are adjusted based on clinical response rather than fixed expectations or predetermined visit counts.
Back pain that limits mobility and disrupts sleep is rarely driven by a single factor. Movement restriction, nervous system sensitivity, and muscular guarding often interact in ways that affect both daytime function and nighttime rest. When acupuncture is used within a careful, assessment-driven framework, it can support symptom management by addressing these contributing systems rather than focusing on pain alone. Outcomes depend on accurate clinical evaluation, realistic expectations, and ongoing reassessment based on how the body responds over time.
If back pain is affecting how you move, rest, or recover, a clinical evaluation with Dr. Jordan Barber can help identify contributing factors, explain why symptoms are persisting, and determine whether acupuncture or related techniques fit appropriately within your care plan.