If you have a nagging ache along your cheekbone, a “tight face” feeling on one side, or temple pressure that shows up with chewing, it can be hard to tell what is actually driving it. When working with a Zygomaticus Major Trigger Point, those symptoms often make more sense because the issue is frequently tied to jaw mechanics and neck tension rather than a simple facial strain. This guide covers how to find the area safely, what referred pain can feel like, how to do a gentle self-release, and when it is smarter to get evaluated in New York City.
A myofascial trigger point is different from general muscle soreness. It is typically a sensitive spot within a taut band of muscle that reproduces familiar symptoms with palpation, often including referred pain.
Soreness is usually diffuse and improves predictably after rest. A trigger point can feel like a small “muscle knot” or nodule, and it may create symptoms that seem out of proportion to how small the area is.
The zygomaticus major is commonly described as a facial expression muscle because it helps lift the mouth corner for smiling. Clinically, it often behaves more like part of a jaw–neck–face coordination loop that helps stabilize the face during chewing, talking, and jaw tracking.
That primary muscle action is only part of the story, because it can also co-contract with jaw and neck muscles to help control facial tension during chewing and speech.
A common pattern is protective overactivity after TMJ irritation, headache cycles, dental work, or upper cervical tension. The temporomandibular joint and the upper cervical spine share close neuromuscular relationships, so irritation in one region can change tone in the other.
In New York City, the triggers are often boring but consistent. Commuting stress, desk ergonomics issues, forward head posture, clenching during focused work, and frequent phone use can keep the system “on,” even when you are not aware of it.
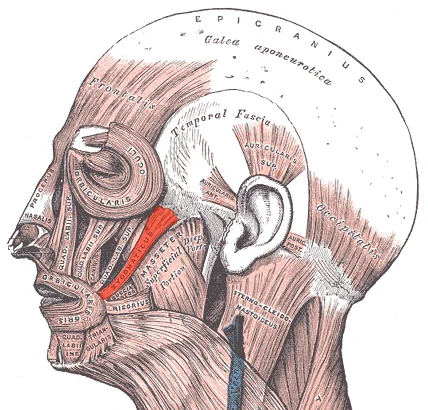
The zygomaticus major runs superficially from the zygomatic bone to the mouth corner. You can think of it as a line along the upper cheek from the cheekbone down toward the corner of the lips.
A nearby muscle, the zygomaticus minor, sits slightly higher and more medial, and it helps elevate the upper lip. If your tenderness is closer to the side of the nose or the upper cheek just below the orbit, you may be palpating zygomaticus minor rather than the zygomaticus major.
Stay superficial and avoid deep pressure near the orbit. If you are close to the eye socket, your pressure is too high or your location is too superior.
For a quick self-check, use a gentle pinch-and-roll along that cheek line. If you find a tender nodule, notice whether it creates local tenderness only or a referral pattern such as temple pressure or a “pulling” sensation around the face.
Referred pain from this region can be surprising. Some people feel cheek pain, some feel temple pressure, and others describe an eye strain feeling or facial tightness that makes the face feel “uneven.”
Jaw tracking can also change when this area is sensitized. You might notice subtle deviation with opening, chewing discomfort, or a sense that the jaw does not glide smoothly.
Symptoms are variable and often asymmetric. Depending on stabilization patterns, the symptoms can be ipsilateral or occasionally contralateral, especially in people with a dominant chewing pattern or habitual neck rotation.
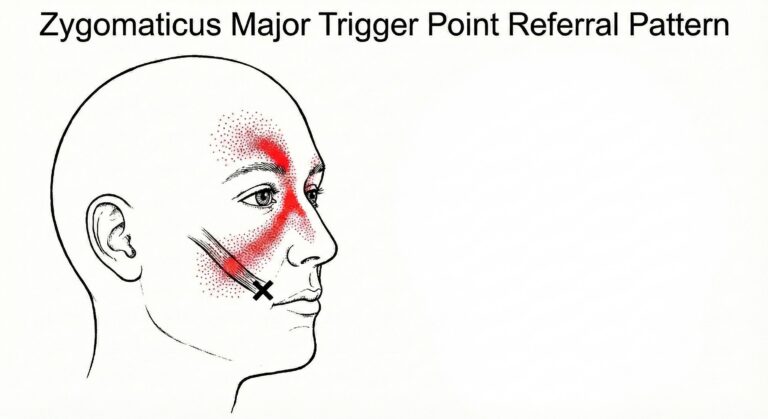
Common symptoms tend to cluster rather than show up alone. Many people notice more than one of the following at the same time.
Root drivers in NYC often involve repetitive low-grade loading rather than a single injury. The most common contributors include bruxism, clenching, altered bite mechanics, post-dental procedure guarding, upper cervical rotation habits, screen time, and forward-head posture that changes cervical posture.
The “tight side” is not always the driver. In many cases, the contralateral side acts as a stabilizer, especially with dominant chewing patterns, chronic neck rotation, or asymmetrical workstation setups.
Red flags matter because facial symptoms can overlap with non-muscular problems. Seek urgent evaluation if you have numbness, facial droop, a sudden severe headache, or vision changes.
After dental work, prolonged mouth opening and temporary occlusal changes can shift how the jaw loads. Even a short period of guarding can recruit facial muscles as a protective strategy, which can perpetuate myofascial pain.
TMJ irritation can also increase background tone in nearby muscles to “splint” the area. That can show up as jaw tension, temple pressure, or a headache pattern that feels like it starts in the face.
In some people, this presents like a tension-type headache, especially when clenching and forward-head posture keep the jaw and upper neck muscles on for hours.
Coordinate care when symptoms persist or your bite feels different for more than a short recovery window. A dentist, a TMJ-focused physical therapy clinician, or a pain management provider can help with diagnosis and a staged plan.
The upper cervical spine is a frequent upstream driver. Sustained upper cervical tension, habitual rotation, and side-bend postures can keep the face and jaw muscles subtly active.
This is why release often does not “hold” if posture and jaw control are unchanged. If the neck keeps feeding the same stabilization demand, the cheek re-engages and the trigger point returns.
Safety first with facial work. Use light pressure only, avoid aggressive digging near the eye, and stop if you feel sharp, electrical, or burning pain that suggests facial nerve irritation or excessive compression.
The goal is to reduce protective tone, not to crush knots. Short bouts followed by reassessment usually work better than long sessions that leave the area sore and reactive.
Pair local self-release with jaw and neck resets for better carryover. This matters because the zygomaticus major often reflects a system problem, not an isolated spot.
Track outcomes that matter functionally. Look for changes in jaw opening symmetry, chewing comfort, temple pressure, and perceived facial evenness.
Wash your hands and keep nails short to avoid irritating the skin. Use a gentle pinch-and-roll along the line from the cheekbone toward the mouth corner.
When you find a tender spot, hold it lightly for 20 to 30 seconds while breathing slowly through the nose. Keep the pressure at a “tender but tolerable” level, then move on rather than staying on one point too long.
Add small jaw movements while holding gentle pressure. Slight open-close motion can teach the muscle to relax during motion and may improve jaw tracking immediately.
Place the tongue lightly on the roof of the mouth and breathe through the nose. Open slowly in a controlled way without forcing range of motion, and stop before clicking or pain.
Keep the neck relaxed and avoid jutting the chin forward. If you notice deviation, reduce the range and aim for smoother control rather than bigger movement.
Do a small chin nod, not a hard tuck, and take 3 to 5 slow breaths. Then add a gentle upper-back extension against the chair to reduce the forward-head posture load.
For phone ergonomics, reduce sustained head rotation while scrolling or on calls. If you are commuting, switch hands or change viewing angles so you are not always rotating the neck the same way.
If symptoms keep returning, in-clinic care can help identify the driver and speed up progress. Common pathways include physical therapy, myofascial trigger point therapy, clinical massage or neuromuscular therapy, acupuncture, and medical evaluation when injections are appropriate.
A good session should include more than spot work. Expect assessment of jaw mechanics, cervical range of motion, chewing dominance, palpation mapping, and a trigger point release protocol that is paired with home exercises.
Dry needling is often informative for this region. Treating the zygomaticus major may change jaw tracking or temple pressure more than local tenderness, which supports the “system” approach rather than a purely local one.
NYC logistics matter because follow-up consistency drives outcomes. Many people choose providers near Midtown East, the Upper West Side, Brooklyn, Downtown Manhattan, or close to their commute so the plan is realistic.
If you are exploring needling-based care, these resources may help:
Trigger point injections are typically considered when persistent myofascial pain does not respond to conservative care. A clinician should review risks, benefits, and expected duration, since relief can vary and is rarely a stand-alone fix.
Clear indications include persistent, reproducible trigger point pain with functional limits, plus failure of a reasonable trial of conservative care such as manual therapy, home release, and jaw and neck retraining.
Coordination with diagnosis is essential before injecting facial pain patterns. Dental pathology, neuralgia, sinus issues, and primary headache disorders should be considered, and many NYC patients coordinate evaluation through systems like Mount Sinai or other hospital networks.
Look for someone who assesses jaw and cervical mechanics, not just the painful cheek. Ask whether they measure change with reassessment metrics like jaw opening symmetry, deviation, and cervical range of motion.
Confirm scope and licensure for the approach you want. Options may include a physical therapy provider, a licensed acupuncturist, a massage therapist offering neuromuscular therapy, or a physician in pain management for medical interventions.
A frequent mistake is chasing the painful cheek only. If the contralateral stabilizer pattern or dominant chewing habits are driving the load, symptoms can persist even with consistent local work.
Another mistake is using too much pressure too often. Facial tissue can sensitize quickly, and aggressive digging may irritate superficial nerves and worsen facial tightness.
Mini case example 1: After dental work, a patient develops guarding and mild jaw deviation. Combined cheek release plus jaw control drills reduces temple pressure and improves jaw tracking within a week, while purely local rubbing did not hold.
Mini case example 2: A desk worker in Manhattan has chronic neck rotation toward a second monitor, plus headaches and cheek tenderness. Symptoms improve after trigger point therapy, but return until the posture micro-reset and desk ergonomics changes are added.
Key takeaways are simple and practical. Treat the loop of jaw + neck + face, reassess function instead of chasing pain, and escalate care if red flags appear or progress stalls.
Get evaluated the same week if you notice any of the following:
It is often related to a myofascial trigger point driven by clenching, bruxism, TMJ irritation, post-dental guarding, or upper cervical tension. It is less commonly a simple “overuse” problem from smiling, even though it is a facial expression muscle.
It runs superficially from the cheekbone, specifically the zygomatic bone, down to the mouth corner. It sits along the upper cheek line where pinch-and-roll and gentle palpation can usually find tenderness if it is involved.
Weakness or poor coordination can affect smiling symmetry and facial tone, and it can change how the face stabilizes during chewing and speech. New drooping, numbness, or rapid changes in facial control should be evaluated promptly to rule out neurological or other medical causes.
The most common areas are typically the neck and shoulders, including upper trapezius and levator scapulae, along with jaw muscles involved in TMJ patterns. Facial trigger points happen as well, but they are less discussed and are often missed when the real driver is cervical posture or jaw mechanics.
Cheek and temple symptoms often feel mysterious because the discomfort is in the face while the driver can be the jaw, the upper cervical spine, or a protective pattern after dental work. If you approach the problem as a coordination issue, using gentle self-release plus jaw tracking and neck resets, you usually get clearer feedback and more durable change.
If symptoms are persistent, worsening, or complicated by bite changes or headaches, an in-person assessment in New York City can help clarify diagnosis and choose the right mix of physical therapy, trigger point therapy, dry needling, acupuncture, or medical options. The goal is not just a less tender cheek, but a calmer system that chews, talks, and holds posture without constantly re-triggering the same spot.




