Hip pain can quietly reshape daily life. Walking becomes cautious. Sitting feels uncomfortable. Sleep positions change without much thought. Many people are told their symptoms come from arthritis, sciatica, or tight muscles, yet imaging findings and lived experience often do not line up simply. For those exploring Acupuncture for Hip Pain from Arthritis, confusion is common when pain patterns shift, fluctuate, or fail to match what scans suggest. Pain may feel deep in the joint one day and spread across the outer hip or glute the next.
This disconnect leads many patients to consider acupuncture, often with unanswered questions. What exactly can it help? How does it work in a clinical setting? Where are its limits?
This article explains how acupuncture is used clinically for hip pain related to joint degeneration, nerve-related referral patterns, and muscular or connective tissue restriction. The goal is clarity, not promises. We focus on why symptoms occur, how treatment decisions are made, and what current evidence supports.
Hip pain is rarely a single-structure problem. The hip sits at the intersection of the spine, pelvis, and lower extremity, and symptoms often reflect interactions between these systems rather than isolated damage.
Pain location does not always equal pain source. The hip is influenced by several overlapping contributors.
Common overlapping contributors include reduced joint motion, nerve sensitization, and protective muscle shortening. This is why arthritis, sciatica, and muscular restriction can feel similar on the surface, even when underlying drivers differ.
Accurate assessment matters before selecting acupuncture techniques. Treating based on diagnosis labels alone often misses why pain persists.
Acupuncture is a licensed medical intervention under New York law. In a clinical pain setting, it is applied based on assessment findings rather than preset protocols or lifestyle models.
Clinical acupuncture differs from wellness-oriented approaches in both intent and execution. Treatment decisions are based on how symptoms behave, not on generalized point recipes.
We consider several factors.
Acupuncture is often combined with other tools when appropriate, including dry needling techniques, myofascial release principles, and neuro-musculoskeletal mapping. These methods are used to target specific contributors identified during evaluation.
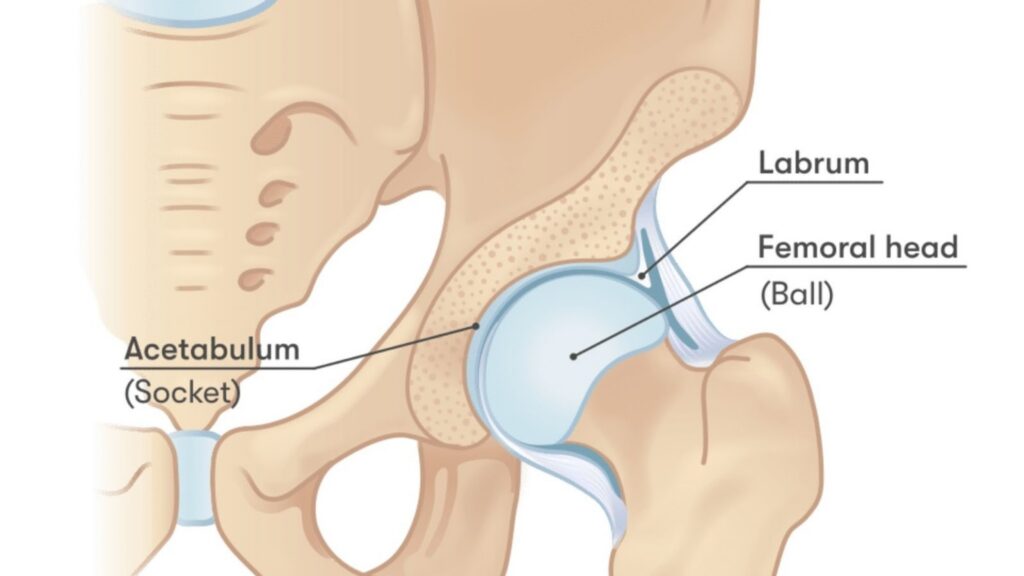
Osteoarthritis involves changes in joint cartilage, altered mechanics, and progressive stiffness. Pain patterns are often load-related, meaning symptoms worsen with standing, walking, or transitions from sitting.
Importantly, imaging severity does not always match pain levels. Some people with advanced radiographic changes report minimal discomfort, while others with mild findings experience significant pain. This suggests that pain signaling, muscle response, and nervous system sensitivity play major roles alongside structural changes.
When we use Acupuncture for Hip Pain from Arthritis, the goal is symptom modulation rather than structural repair. Acupuncture may help by influencing pain signaling pathways, improving surrounding muscle function, and supporting joint movement tolerance.
It does not regenerate cartilage or reverse joint degeneration. Instead, it aims to reduce the nervous system’s amplification of joint stress and improve how the hip is supported during movement.
Research on acupuncture for osteoarthritis, including hip and knee arthritis, suggests modest symptom relief for some patients. Systematic reviews have found improvements in pain and function compared with sham or usual care, though results vary widely between studies.
The evidence supports symptom management, not joint regeneration. Limitations of existing studies include variable treatment protocols, short follow-up periods, and differences in patient selection. These factors make it difficult to predict individual response.
Outcomes often depend on mechanical contributors beyond the joint surface itself. When muscle control, pelvic mechanics, or nerve sensitivity drive pain, acupuncture may be more helpful than when symptoms are dominated by advanced structural limitation.
Response may be limited when there is severe mobility restriction, advanced structural collapse, or pain driven primarily by load intolerance rather than neural input. In these cases, acupuncture may still play a supportive role, but expectations should remain realistic.
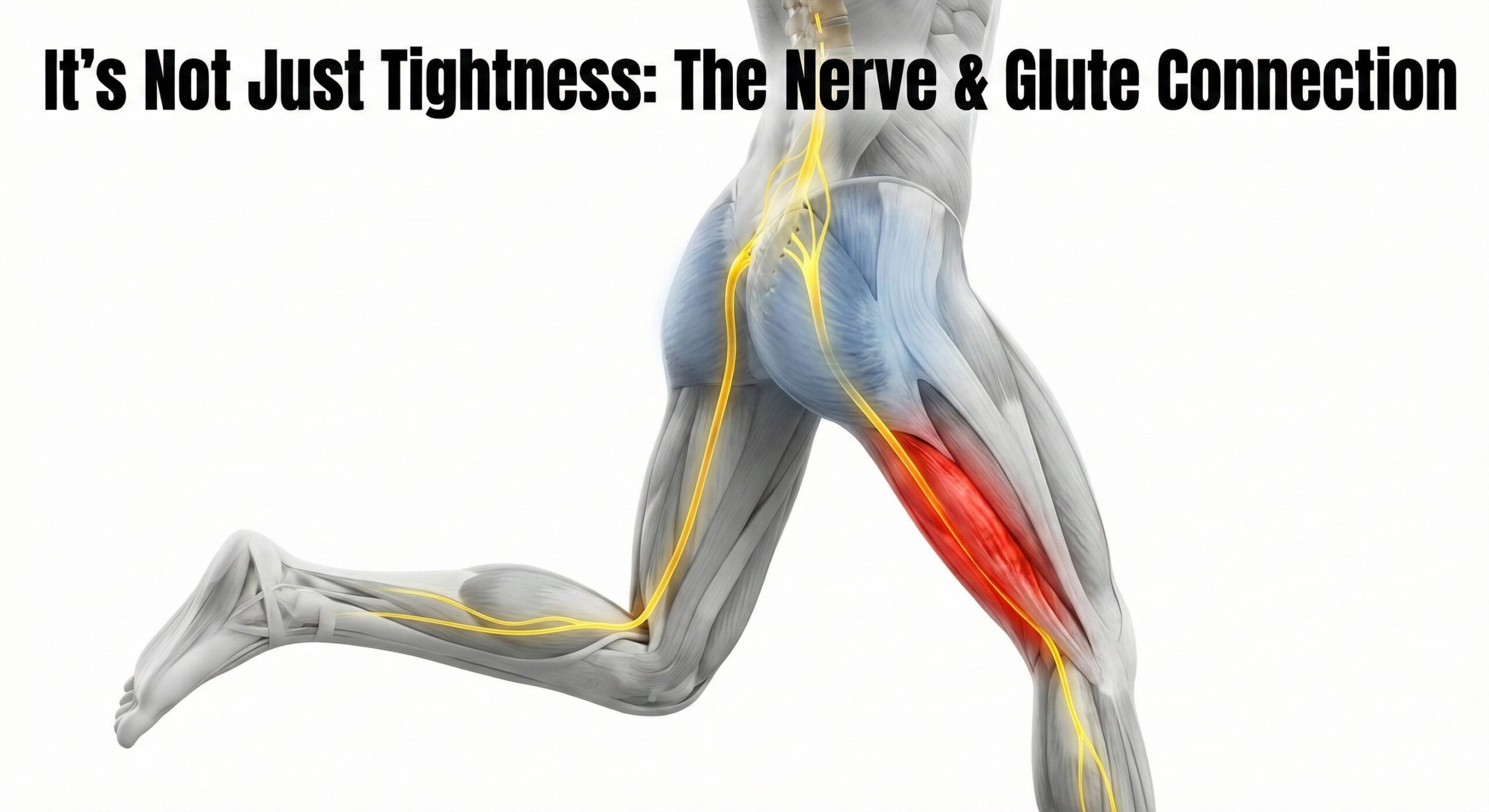
Sciatic symptoms originate from lumbar nerve roots but often present away from the spine. Referred pain commonly appears in the lateral hip, gluteal region, or posterior thigh. This leads many patients to believe the hip joint itself is the problem.
Nerve-related pain is frequently mislabeled as hip arthritis, particularly when imaging shows age-related joint changes that may not be clinically meaningful.
When using Acupuncture for Hip Pain from Sciatica, the clinical focus shifts toward nerve sensitivity and surrounding muscle response. Acupuncture may help by addressing protective muscle tone around irritated nerves and supporting central pain modulation within the nervous system.
It is important to differentiate nerve irritation from true nerve compression. Acupuncture does not decompress discs or reverse spinal stenosis, but it may influence how the nervous system processes and responds to irritation.
Studies examining acupuncture for radicular or sciatic pain suggest potential short-term symptom reduction for some individuals. Results vary based on the underlying cause, such as disc involvement or spinal narrowing, and on symptom duration.
Long-standing compression or progressive neurologic deficits tend to respond less predictably. This reinforces the need for accurate diagnosis before deciding whether acupuncture is appropriate.
Muscular and connective tissue restriction is a common contributor to hip pain, particularly in people who sit for long periods or perform repetitive activities. Key muscles often involved include the gluteus medius and minimus, deep hip rotators, and the iliopsoas.
When these muscles shorten or guard, they can alter joint mechanics and irritate nearby nerves, producing pain that mimics joint or nerve pathology.
In cases of Acupuncture for Hip Pain from Tight Muscles, treatment may involve trigger point deactivation, improved local circulation, and reduction of protective guarding. Dry needling techniques are sometimes used alongside traditional acupuncture to address focal muscle dysfunction.
The intent is not relaxation alone but restoration of more normal muscle behavior during movement.
Muscle-focused treatment tends to be most effective when pain is clearly linked to movement patterns, symptoms are reproducible with muscle testing, and there is no significant joint degeneration dominating the picture.
Hip pain treatment begins with evaluation, not assumptions. We rely on movement testing, neurologic screening, and load response evaluation to determine primary contributors.
This process often reveals that meaningful drivers lie beyond the hip itself. Treatment may include lumbar, pelvic, or even foot and ankle considerations when they influence hip mechanics.
Treatment plans follow a general structure rather than fixed timelines. An initial evaluation phase establishes working hypotheses. Short-term response monitoring helps determine whether acupuncture is influencing symptoms in a meaningful way.
Plans are adjusted based on symptom behavior rather than predetermined visit counts. Endless treatment plans are avoided when response is limited or absent, and alternative strategies are discussed.
Acupuncture is generally well-tolerated when provided by licensed professionals. Possible mild effects include temporary soreness or fatigue. Serious adverse events are rare when proper clinical standards are followed.
There are situations where coordination with or referral to other providers is appropriate. Acupuncture does not replace emergency or surgical care and should be part of an informed care plan.
Individuals with progressive neurologic deficits, acute trauma, or undiagnosed systemic conditions require medical evaluation before considering acupuncture. Red flags should always be addressed through appropriate medical channels.
How long before improvement is noticed?
Response varies. Some people notice changes within a few sessions, while others require more time to assess the effect.
Does acupuncture work alone or with other care?
It is often most effective when integrated with other appropriate care strategies.
How are outcomes measured clinically?
Changes in pain behavior, movement tolerance, and functional capacity guide decisions.
What if symptoms do not change?
Lack of response prompts reassessment and discussion of alternative options.
Hip pain is complex and often multifactorial. Acupuncture can play a meaningful role when it is used selectively and guided by clinical reasoning rather than protocols. Outcomes depend on accurate diagnosis, realistic expectations, and how each individual’s anatomy and nervous system respond to care.
If you are experiencing persistent hip pain and want a clear, anatomy-based explanation of what may be contributing to it, a clinical evaluation with Dr. Jordan Barber can help clarify underlying drivers and determine whether acupuncture or related techniques are the appropriate next steps.