
If your jaw feels “stuck,” your ear feels full, or chewing suddenly seems harder, it is easy to assume the problem must be your teeth or your ear. When working with Medial Pterygoid Trigger Points, those symptoms often make more sense because this deep jaw muscle can refer pain and pressure into places that do not feel like “muscle pain” at all. This guide covers the medial pterygoid muscle’s referral pattern, simple screening, and safe ways to calm the system without irritating sensitive intraoral tissue.
If you have seen a trigger point referral map for the medial pterygoid, the goal here is to help you match that pattern to real-world symptoms and then choose the lowest-risk steps to reduce irritation.
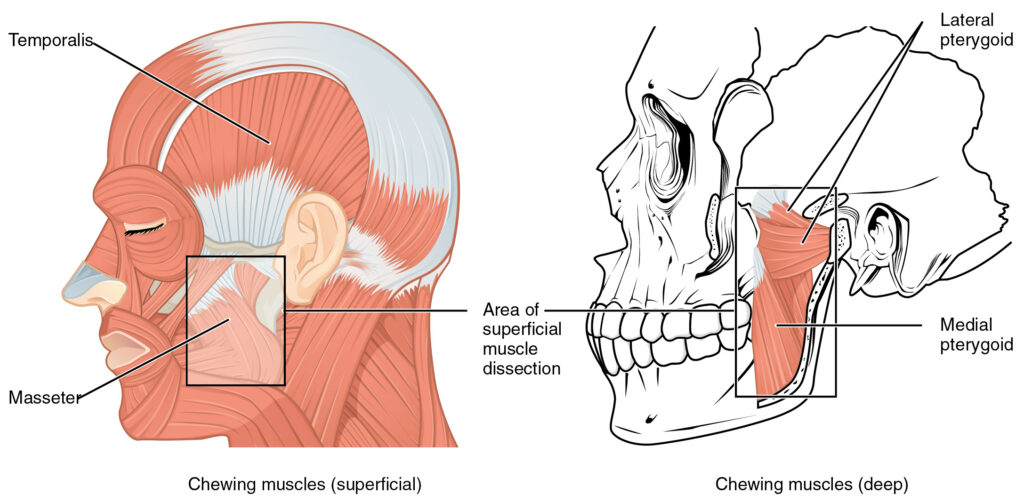
The medial pterygoid muscle is a deep jaw muscle on the inner side of the mandible that helps elevate the jaw (closing) and assists side-to-side movement. It is one of the pterygoid muscles, working in coordination with the lateral pterygoid, masseter, and temporalis to guide bite mechanics and jaw tracking.
Trigger points are hypersensitive spots within a taut band of muscle that can create local tenderness and referred pain. When trigger points contribute to broader, persistent symptoms, the pattern is often discussed under myofascial pain or myofascial pain syndrome, especially when multiple muscles and regions become sensitized together.
In temporomandibular disorders (TMD), symptoms can feel dental, ear-related, or throat-related rather than like straightforward jaw pain. That is one reason TMJ or temporomandibular joint complaints can be confusing, since the temporomandibular joint itself may not be the only driver.
A key clinical nuance is that the medial pterygoid often behaves like a stabilizer reacting to asymmetry, not just a “stress muscle” from clenching. In many cases, the neuromuscular pattern is trying to keep the mandible centered despite changes in occlusion, cervical mechanics, or airway function.
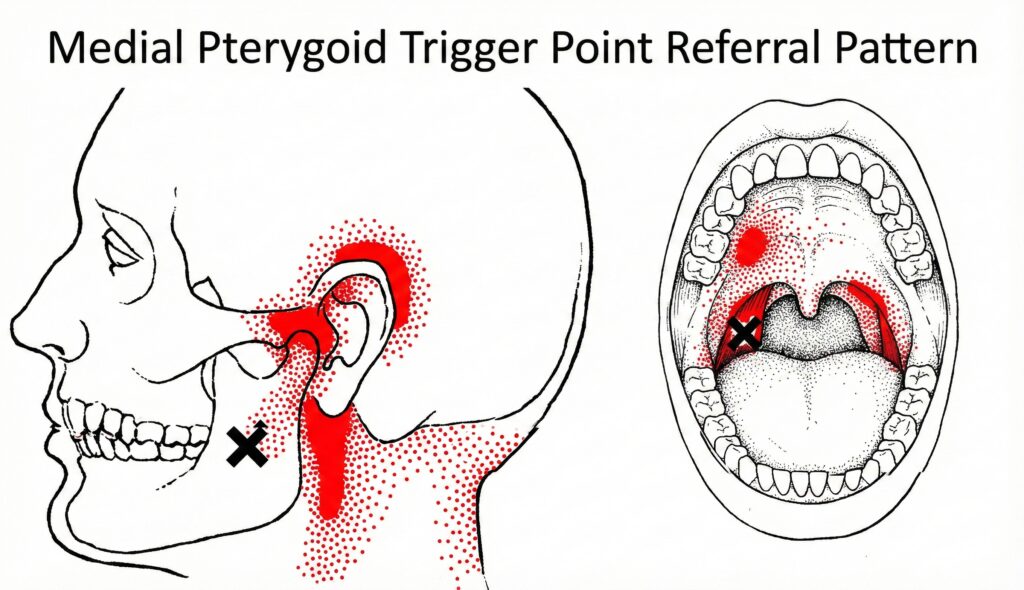
A classic referral pattern from this muscle includes a deep ache behind or below the TMJ, along with deep ear pressure or ear fullness. Some people also notice throat discomfort, posterior mouth discomfort, or a vague pharynx irritation that does not match a typical sore throat.
Less obvious signs include altered bite perception, like the teeth “don’t meet the same” or the bite feels off-center. You may also notice changes in neck tone or head balance, as if your head sits differently over your shoulders after chewing or talking.
Clenching and bruxism can contribute, but asymmetry is often the bigger story. Unilateral chewing, old dental work, subtle occlusal changes, postural asymmetry, and cervical spine mechanics can all increase stabilizing demand on the medial pterygoid.
Breathing pattern and tongue posture matter more than most people realize. If nasal breathing is limited or tongue function is poor, the system may recruit jaw and neck muscles as a workaround, keeping the medial pterygoid “on” as part of a stabilization strategy.
Hallmark symptoms that commonly fit this presentation include:
It is also important to separate this from red flags that need medical or dental evaluation first. Seek urgent or same-day evaluation for suspected infection, acute dental pathology, neuralgia-type “electric” facial pain, sudden hearing loss, significant trauma, facial swelling, fever, or rapidly worsening neurologic signs.
A practical way to screen is a simple symptom cluster approach:
Side dominance matters. The painful side is not always the primary stabilizing side, especially when unilateral chewing or cervical rotation patterns have been present for years.
These checks are not a diagnosis, but they can help you decide whether this pattern is plausible.
Jaw motion check:
Habit check:
Refer out when symptoms persist longer than 2 to 4 weeks despite conservative care, or sooner if symptoms are severe. Significant jaw locking, progressive limitation, or neurologic signs should be evaluated promptly.
Because symptoms can mimic dental or ear pathology, coordination with dentistry, ENT, or a clinician specializing in orofacial pain is often the fastest path to clarity. If you are exploring a TMJ-focused pathway, see TMJ Dysfunction for condition-specific guidance and treatment options.
The goal is down-regulation and improved jaw mechanics, not aggressive digging into deep tissues. With this muscle, “more pressure” commonly backfires by increasing protective tone and sensitizing the area.
Safety comes first with any intraoral release. Intraoral work can irritate tissue, and it should be done with clean hands and ideally gloves, while avoiding sharp nails and excessive pressure.
Stop immediately if you notice sharp pain, dizziness, nausea, gagging that escalates, or a clear symptom spike in ear pressure, jaw locking, or headache. If symptoms flare after self-treatment, that is useful information that your dose was too high or the driver is elsewhere, such as cervical spine irritation or occlusion changes.
Sequence matters:
Track outcomes in functional terms. Pay attention to bite feel, ear pressure, jaw opening, and neck ease, since changes can be immediate and meaningful even if pain takes longer to settle.
Use nasal breathing and a calm jaw rest position. Keep the tongue posture light on the palate, teeth apart, and lips closed, with the jaw hanging without effort.
As you breathe, reduce accessory neck tension. Let the sternocleidomastoid and upper trapezius soften so the cervical spine is not bracing, since neck bracing can increase jaw elevator tone.
Start with the masseter, since calming superficial jaw elevators often reduces protective tone before you consider anything deeper. Use a light, sustained pressure for 30 to 60 seconds on tender spots, then reassess jaw opening and jaw tracking.
You can also work the submandibular region gently, but avoid pressing aggressively under the jaw angle. Too much pressure near the mandibular angle can irritate sensitive tissue and may increase guarding rather than reduce it.
If you choose intraoral release, keep the dose low. Use a clean, gloved thumb or finger to contact the inner jaw near the back molars, applying gentle compression rather than scraping.
Stay within 2 to 3 out of 10 discomfort, and avoid hunting for intense pain. Do 2 to 3 holds of 20 to 30 seconds, then reassess jaw opening, bite perception, and ear pressure.
If your jaw feels more guarded afterward, stop and switch back to breathing, external work, and jaw motion retraining. If you have a history of jaw locking, significant TMJ irritability, or high anxiety around gag reflex, it is usually better to skip intraoral self-treatment and work with a clinician.
The contralateral stabilizer concept explains why treating the non-painful side sometimes produces the biggest shift. If the system is trying to center the mandible, the opposite medial pterygoid may be overworking to control deviation and stabilize occlusion.
Pattern recognition helps guide this. Unilateral chewing, dental work that subtly changed occlusion, and cervical mechanics such as habitual cervical rotation can shift load across the jaw and neck, even when symptoms show up on only one side.
With skilled care, expected responses can include changes in bite perception, reduced ear pressure, smoother jaw tracking, and a noticeable shift in neck tone. Many people also report that their head feels more balanced over their shoulders, which is a clue that the jaw and cervical spine are being treated as a linked system.
Durability follows a principle that surprises people. Results hold best when cervical mechanics and airway and tongue function are addressed, since forward head posture and an altered breathing pattern can re-recruit the jaw elevators.
Dry needling and manual therapy can reduce guarding and improve jaw excursion quickly in the right patient. It is also normal to feel localized soreness for 24 to 48 hours afterward, particularly when myofascial trigger point release is performed in sensitized tissue.
Good treatment planning includes reassessment of jaw tracking, cervical spine posture, and functional tolerance for chewing, not only pain scores. If you are considering this route, see dry needling trigger point acupuncture in nyc the science of resolving chronic pain for an overview of how dry needling is used clinically.
Forward head posture and limited upper cervical rotation can keep jaw elevators active, even when you are not chewing. When the cervical spine cannot move well, the jaw often compensates during talking, swallowing, and head turning.
Tongue posture and nasal breathing support mandibular stability. Better airway function reduces compensatory clenching, and it often lowers baseline tone in the pterygoid muscles over time.
Common mistakes that slow progress include:
Special cases deserve extra caution. For TMJ care during pregnancy, prioritize gentle positioning, nasal breathing, heat, posture support, and clinician-guided options, since hormonal changes and sleep disruption can increase sensitivity and clenching.
A workable home plan is short and frequent. Two to three daily resets of 60 to 90 seconds often outperform long, intense sessions that irritate tissue, especially when self-treatment is involved.
The big takeaway is that the medial pterygoid often acts like a checkpoint for whole head-neck-jaw coordination. When symptoms keep returning, it is usually a sign that occlusion, cervical mechanics, breathing pattern, and tongue posture still need attention, not that you failed to “release” one muscle.
Use function-based markers to judge progress:
Start with nasal breathing and a relaxed jaw rest position, keeping the tongue lightly on the palate with teeth apart and lips closed. Then use gentle external work on the masseter and submandibular region to reduce overall jaw elevator tone before considering intraoral release.
If you use intraoral pressure, keep it light and brief, using gentle compression rather than scraping. Stop if symptoms spike, especially ear pressure, nausea, dizziness, or increased jaw locking.
Symptoms often include a deep jaw ache, pain behind or below the TMJ, and ear pressure or ear fullness that does not feel like a typical ear infection. Many people also notice throat discomfort or posterior mouth discomfort, chewing fatigue, limited mouth opening, and a changed bite feel.
Jaw clicking can coexist with this pattern, and jaw locking can occur when guarding increases. The referral pattern can make it feel like a tooth, ear, or throat issue rather than a jaw muscle issue.
Prioritize low-risk strategies, including jaw rest position practice, nasal breathing, gentle heat, and posture support to reduce forward head posture strain. Clinician-guided manual therapy can be appropriate, but aggressive intraoral techniques are usually not the first choice.
Ask your OB, midwife, or prenatal care team about safety, especially if you are considering any new treatment. If symptoms are persistent or severe, coordinate care with a provider experienced in TMD and orofacial pain.
Clenching and bruxism can contribute, but asymmetry is a common driver. Unilateral chewing, occlusal changes after dental work, and cervical mechanics problems can increase stabilizing demand on the pterygoid muscles.
Breathing pattern and tongue posture also matter. When airway function is compromised and nasal breathing is limited, the jaw and neck may compensate, reinforcing a neuromuscular pattern that keeps the pterygoids active.
Medial pterygoid involvement is easy to miss because it can present as ear pressure, throat discomfort, or a strange change in bite perception rather than obvious jaw pain. The most reliable improvements come from a safe sequence: calm breathing and cervical position first, gentle external release next, minimal-dose intraoral release only if needed, and then movement retraining so the system stops re-bracing.
If your symptoms persist, worsen, or include significant jaw locking or progressive limitation, a targeted evaluation can clarify whether the primary driver is the jaw, the cervical spine, occlusion, or a broader TMD pattern. When the plan addresses the whole head-neck-jaw system, relief tends to be faster, more predictable, and more durable.




